-
Die Universität
- Herzlich willkommen
- Das sind wir
- Medien & PR
-
Studium
- Allgemein
- Studienangebot
- Campusleben
-
Forschung
- Profil
- Infrastruktur
- Kooperationen
- Services
-
Karriere
- Arbeitgeberin Med Uni Graz
- Potenziale
- Arbeitsumfeld
- Offene Stellen
-
Diagnostik
- Patient*innen
- Zuweiser*innen
-
Gesundheitsthemen
- Gesundheitsinfrastruktur
Case of the Month
April 2024
Subtotal colectomy in a 56-year-old male with aortic dissection.
Diagnosis
Sevelamer-induced colitis.
Comment
A 56-year-old male patient underwent emergency reconstructive vascular surgery due to Stanford A type aortic dissection. Dissection started in the ascending aorta and spread to the iliac arteries. Postoperatively, the patient suffered from renal failure, sepsis and melena. Laboratory findings showed elevated PO43+ values in blood, going up to 6.25 mg/dl (normal range 2.60-4.50) and lowered Ca2+ values, going down to 1.74 mmol/L (normal range 2.20-2.65), therefore sevelamer was prescribed. Multiple colonic ulcers were seen on endoscopy, while the upper endoscopy was unremarkable. Because of continuous bleeding, the patient underwent explorative laparotomy and finally subtotal colectomy.
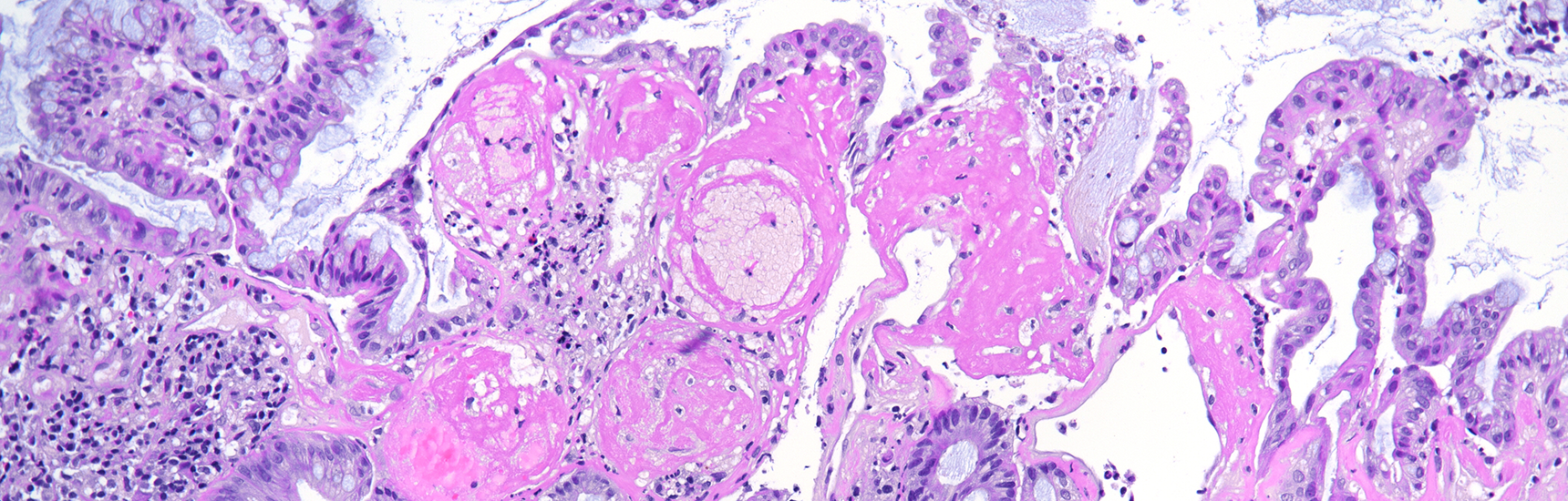
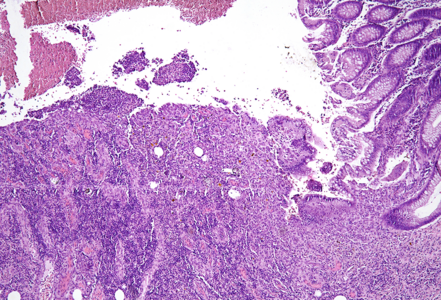
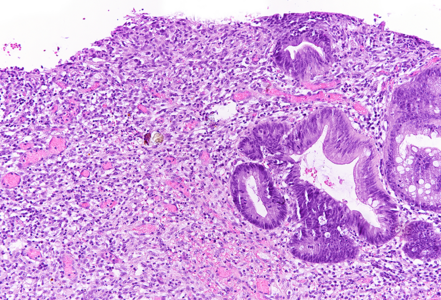
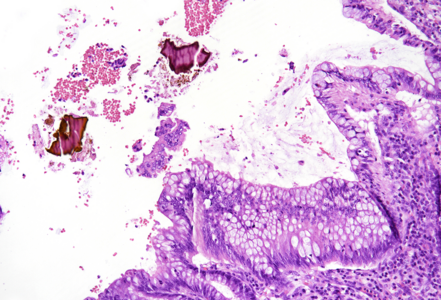
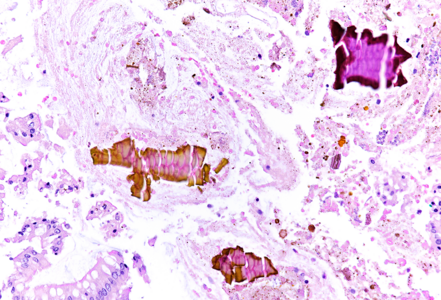
On macroscopy, multiple ulcers were visible on the mucosa of the colon. Histology showed ulcers with prominent granulation tissue, reaching the muscular wall of the bowel. They were surrounded by colonic mucosa with regenerative architectural changes (Panels A-B). In the ulcers and on the surface mucosa, yellow-pink polygonal foreign material with scale-like appearance was seen, which corresponded to the given sevelamer drug (Panels C-D).
Sevelamer-induced GI side effects are complications which can affect GI tract from oesophagus to the rectum and may cause nausea, vomiting, diarrhoea, gastroesophageal reflux, dyspepsia, abdominal pain, constipation, obstruction, flatulence and perforation. Histologically visible side effects are mucosal injury with acute inflammation, necrosis, and ulceration. In our case, mucosal injury was most probably caused by a combination of two factors, which are ischemic injury due to aortic dissection that was aggravated by the drug effect.
It is important to have these side effects in mind when dealing with patients suffering from acute or chronic renal failure. If detected histologically, the presence of (putative) sevelamer-induced mucosal injury needs to be reported urgently to the clinitians to avoid additional complications in other parts of the bowel, such as perforation and peritonitis.
For further reading
- Swanson BJ, Limketkai BN, Liu T-C et al.: Sevelamer Crystals in the Gastrointestinal Tract (GIT). A New Entity Associated with Mucosal Injury.; Am J Surg Pathol 2013;37:1686-1693.
- Gonzalez RS, Lagana SM, Szeto O, Arnold CA: Challenges in Diagnosing Medication Resins in Surgical Pathology Specimens: A Crystal-Clear Review Guide. Arch Pathol Lab Med. 2017 Sep;141(9):1276-1282.
- Nambiar S, Pillai UK, Devasahayam J et al.: Colonic Mucosal Ulceration and Gastrointestinal Bleeding Associated with Sevelamer Crystal Deposition in a Patient with End Stage Renal Disease. Case Rep Nephrol. 2018; 2018: 4708068.
- Lai T, Frugoli A, Barrows B, Salehpour M: Sevelamer Carbonate Crystal-Induced Colitis; Case Rep Gastrointest Med. 2020; 2020: 4646732.
Presented by
Dr. Sara Hrg, Zagreb, Croatia, Dr. Cord Langner, Graz, Austria.